When you hear "nonverbal autism," it's easy to picture a child who simply doesn't speak. But that's not the whole story. The reality is far more complex and interesting—it’s not an absence of communication, but a different way of communicating that often uses actions, sounds, and gestures instead of spoken words.
Unpacking What Nonverbal Communication Really Means
For many parents, getting a nonverbal or minimally verbal diagnosis can feel overwhelming. The key is to reframe what "nonverbal" actually means. It doesn't mean your child has nothing to say, and it certainly doesn't reflect what they understand. It just means spoken language isn't their primary tool for expression.
Think about it this way: everyone uses nonverbal cues like a nod, a smile, or a wave. For some autistic individuals, these channels are their main language. Their communication might look like:
- Leading a parent by the hand to the kitchen to show they're hungry.
- Making specific sounds to express joy or frustration.
- Pointing to objects or pictures to make a choice.
- Turning their body away to signal they need a break.
A Different Communication Profile
Seeing these actions as language is the first step toward building a bridge. It requires a shift in focus—from listening for words to observing for meaning. To dig deeper into how language and non-verbal cues function in real-world contexts, exploring methods like discourse analysis can offer valuable frameworks. Ultimately, it’s about learning your child's unique language instead of expecting them to conform to yours.
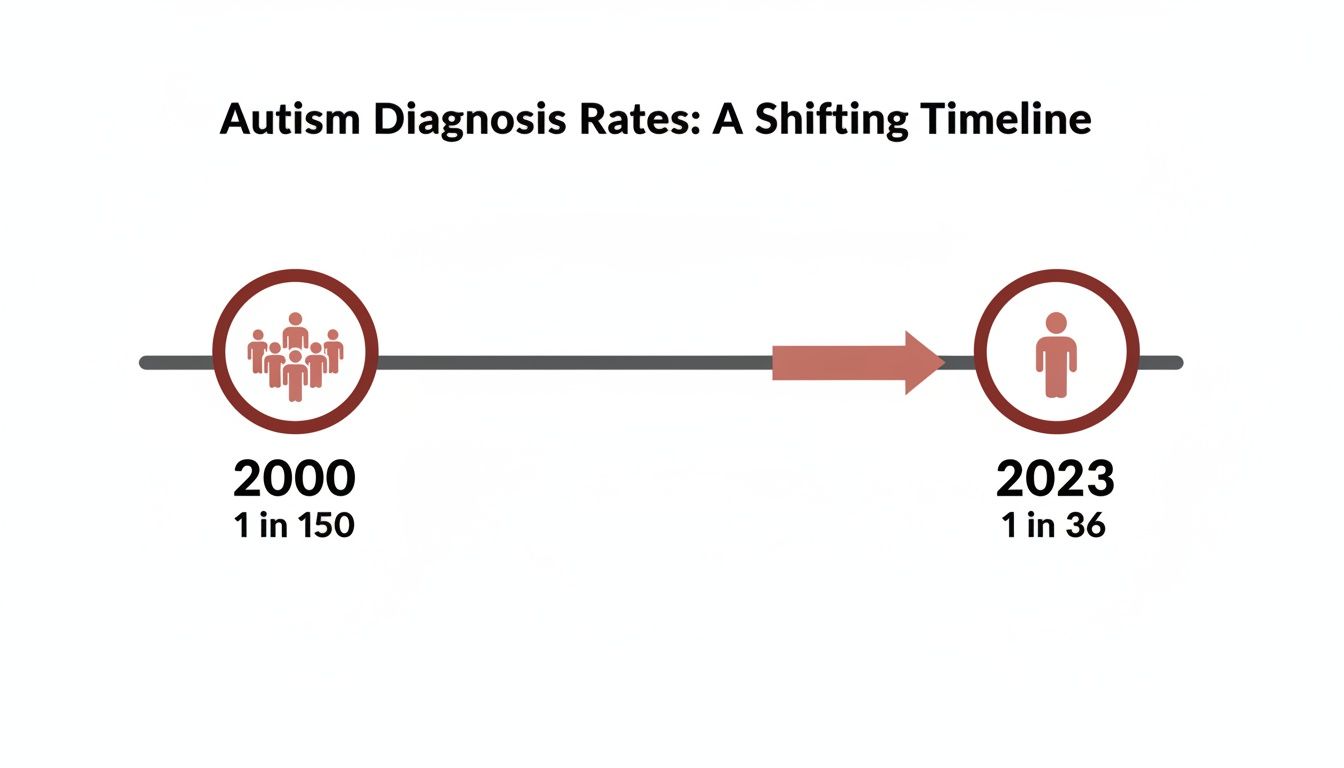
This isn't a rare occurrence. Statistics show that between 25-30% of children with autism spectrum disorder are nonverbal or minimally verbal, meaning they use fewer than 30 functional words. This underscores how vital it is to recognize and support every form of expression.
The table below offers a snapshot of how communication can differ, helping to clarify these distinct profiles.
Understanding Communication Differences in Autism
| Communication Aspect | Typical Verbal Development | Common in Nonverbal Autism |
|---|---|---|
| Primary Expression | Spoken words and sentences form the core of communication. | Gestures, sounds, body language, and pointing are primary. |
| Language Acquisition | Follows a predictable path from babbling to words to sentences. | May be non-linear; some may use echolalia or scripting. |
| Social Interaction | Relies heavily on verbal back-and-forth, questions, and answers. | Initiated through physical actions (e.g., giving an object). |
| Expressing Needs | "I'm hungry" or "I want juice." | Leading a person to the fridge or pointing at a cup. |
| Showing Emotion | Verbal labels like "I'm happy" or "I'm sad." | Vocalizations (joyful sounds) or physical actions (stimming). |
This comparison isn't about deficits; it's about recognizing different, equally valid ways of connecting with the world.
As awareness has grown, so have diagnosis rates, highlighting the need for more inclusive communication strategies.
The leap from 1 in 150 children in 2000 to 1 in 36 in 2023 shows just how many families are navigating this. These communication challenges sometimes overlap with other conditions, which you can learn more about in our guide to Social Communication Disorder.
A nonverbal diagnosis isn’t an endpoint. It’s the starting point for discovering the right tools and strategies that will allow your child's unique voice—in whatever form it takes—to be heard clearly.
When you presume competence and genuinely seek to understand, you create an environment where your child feels seen and valued. This foundation of trust is the key to helping them express their needs, thoughts, and personality more fully.
Recognizing Communication Clues Across Different Ages
The way an autistic child communicates nonverbally isn't static—it shifts and evolves as they grow. A subtle difference you might notice in a toddler can blossom into a more distinct communication style by the time they're in school or navigating their teen years.
Learning to spot these patterns isn’t about checking off a list of deficits. It’s about learning to tune into your child's unique frequency at every stage of their development, moving from just listening for words to watching for meaning.
Toddlers and Preschoolers
In the very early years, the differences often show up in the fundamental building blocks of social connection. For instance, a neurotypical toddler might point excitedly at a passing airplane to share the moment with you. An autistic toddler, on the other hand, might simply guide your hand toward something they want, often without making direct eye contact.
Some common patterns you might see in this age group include:
- Atypical Eye Contact: It might be fleeting, indirect, or focused on a person’s mouth instead of their eyes.
- Limited Gestures: You may notice an absence of typical gestures like waving "bye-bye," pointing to things they find interesting, or clapping along with a song.
- Unique Vocalizations: Instead of babbling that mimics the rhythm of speech, their sounds might be more repetitive or used for self-soothing rather than trying to engage.
- Unusual Object Use: A child might become intensely focused on one part of a toy—like spinning the wheels of a car—instead of using it for pretend play.
These aren't just missed milestones; they're early signs of a different neurodevelopmental path. Recognizing them is the first step toward getting the right support.
School-Aged Children
Once children start school, the social world gets a lot more complicated. This is often when differences in nonverbal communication become more obvious. An autistic child might have a hard time interpreting the subtle social signals from their peers, like reading a facial expression or catching sarcasm.
For many autistic children, the unspoken rules of playground politics are like a foreign language without a dictionary. They often want to connect but may not have the innate tools to navigate these complex social exchanges.
At this stage, you might observe:
- Difficulty with Personal Space: They might stand too close to others or seem unaware of typical social boundaries.
- Literal Interpretation: A teacher’s casual phrase like "it's raining cats and dogs" could cause genuine confusion or even distress.
- Challenges with Turn-Taking: Conversations can feel one-sided, frequently circling back to the child’s specific, intense interests.
- Flat Affect: Their facial expressions or tone of voice may not seem to match the emotion they're feeling inside, which can be easily misinterpreted by others as boredom or rudeness.
Teenagers and Young Adults
The teenage years bring a new level of focus on peer relationships and figuring out who you are. For autistic teens, this period can be especially tough as nonverbal cues become even more subtle and layered. They may feel a profound sense of social isolation, even when they're surrounded by people.
This is a critical time when understanding and support can make all the difference. While some teens learn to "mask" their autistic traits to blend in, this is mentally and emotionally exhausting. The underlying differences are still there, and they require a compassionate, informed approach. If these patterns sound familiar, it’s worth learning more about the common signs of autism in teens.
In this age group, communication patterns may include:
- Scripting or Echolalia: They might repeat lines from movies or TV shows to express an emotion or to help them navigate a social situation.
- Monologuing: Conversations can be dominated by their special interests, and they may struggle to shift topics or engage in a back-and-forth dialogue.
- Physical Stimming: Repetitive movements like hand-flapping or rocking can become more noticeable during moments of high stress or excitement.
Understanding these clues across the different stages of childhood is the first real step toward becoming an effective advocate. It gives you the knowledge to seek a professional evaluation that can provide clarity and unlock the right resources to help your child truly thrive.
Uncovering Your Child's Hidden Understanding
One of the biggest "aha" moments for parents is realizing that "nonverbal" doesn't mean "non-understanding." There's a world of difference between receptive language (what a child actually understands) and expressive language (what they're able to say or show). When we miss this distinction, it can lead to a ton of frustration for everyone involved.
Think of it like this: Imagine a super-powerful computer with a brilliant processor, packed with information and ready to solve complex problems. The only catch? Its keyboard and mouse are broken. The computer gets every command, but it has no way to output the answers. This is a great way to think about nonverbal communication and autism; the processing is happening on the inside, even when the external expression is limited.
This gap isn't just a theory; it's a well-documented reality. Research shows that about 25% of nonverbal children with autism have receptive language skills that are significantly stronger than their expressive ones. In one landmark study, many of these kids weren't using two-word phrases at age 4. But by age 8, an incredible 70% hit that milestone, and nearly half were speaking fluently. This just goes to show the immense potential that's often waiting just beneath the surface.
Presuming Competence: A Foundational Mindset
This brings us to a crucial guiding principle in the autism community: presume competence. It's a simple but profound idea—always assume your child understands what's being said to them and about them, even if they don't show any outward sign that they're taking it in.
Adopting this mindset changes everything. It shifts how you speak to and interact with your child, creating an environment built on respect and encouragement instead of one focused on what they can't do.
When you presume competence, you stop testing and start connecting. You provide your child with the dignity of being understood, which is the foundation of all true communication.
This perspective shift is empowering. It encourages you to seek out assessments that look beyond what your child can say. A proper evaluation can uncover a child's true cognitive abilities, separate from their speech challenges, giving you a much clearer picture of their strengths.
Looking Beyond Words
Once you start to recognize this hidden comprehension, you'll begin to tune into the more subtle ways your child is already communicating. You'll start to see the intelligence behind their actions and learn to speak their unique language. A fantastic resource for parents and educators looking to hone this skill is understanding unspoken questions, which offers fresh perspectives on interpreting these messages.
By acknowledging that a silent child is often an observant and intelligent child, you can focus on building bridges to their inner world. The goal changes from "making them talk" to "giving them the tools to express what they already know." This is where strategies like Augmentative and Alternative Communication (AAC) and targeted therapies become so essential—they provide the "keyboard" for a mind that's ready and waiting to communicate.
Practical Strategies for Building Communication Bridges
Understanding that a nonverbal child has a rich inner world is the first step. The next, and most crucial, is building the bridge to it. This means shifting our focus from trying to teach them our way of communicating to learning theirs—and then providing tools that actually work for them. These strategies aren't about "fixing" a communication difference; they’re about forging genuine connections and honoring every single attempt to express a thought, need, or feeling.
The journey starts when we recognize that communication is so much more than just spoken words. For many autistic individuals, a simple glance, a specific gesture, or even leading you by the hand is a deliberate act of communication. The key is to validate these attempts and build upon them with patience and consistency, turning moments of frustration into opportunities for connection.
Introducing Augmentative and Alternative Communication
When speech isn't the primary way a child expresses themselves, Augmentative and Alternative Communication (AAC) opens up other pathways. It’s best to think of AAC not as a replacement for speech, but as a powerful support system. It gives your child a reliable voice, which can dramatically reduce frustration and empower them to participate more fully in their world.
AAC isn't a one-size-fits-all solution; it exists on a spectrum from simple, low-tech tools to sophisticated, high-tech devices.
-
Low-Tech AAC: These are simple, non-electronic options that make a great starting point. This could be pointing to pictures on a communication board, using a Picture Exchange Communication System (PECS) where a child hands you a picture of what they want, or learning basic sign language.
-
High-Tech AAC: This category includes dedicated speech-generating devices (SGDs) or specialized apps on a tablet. These tools allow a user to press a button with a picture or word, and the device speaks the message aloud. They can be customized with thousands of words, allowing for incredibly complex sentence building.
The goal is to find the system that best matches your child's physical abilities and cognitive skills. For example, a child with fine motor challenges might find a large button on a tablet far more effective than trying to form intricate hand signs.
A common myth is that AAC stops a child from learning to speak. Research consistently shows the opposite is true. By reducing the pressure to speak and providing a consistent model for language, AAC can actually support the development of verbal skills.
Creating a Communication-Rich Home Environment
The tools are important, but the environment where they're used is just as critical. A communication-rich home is one where every attempt to communicate—no matter how small—is celebrated and supported. It’s about creating countless natural opportunities for your child to use their voice, whatever form it takes.
One of the most powerful strategies is modeling. This simply means you use the AAC system yourself when you talk to your child. If you want to ask them if they want a snack, you would say the words aloud while also pointing to the "snack" icon on their device. This shows them how the tool works in a natural, everyday context, not just during therapy sessions.
Communication Support Strategies At-a-Glance
To help put this all together, here is a quick-reference table breaking down some key strategies, their purpose, and how you can start implementing them today.
| Strategy Type | Description | Practical Example |
|---|---|---|
| Visual Supports | Using pictures, schedules, or charts to make routines predictable and reduce anxiety. | A visual schedule with pictures for "get dressed," "eat breakfast," and "get in car" to help your child understand the morning routine. |
| Modeling AAC | Using the child's AAC system to communicate with them, demonstrating its function. | Tapping the "all done" icon on their device while saying, "We are all done with dinner," to end a meal. |
| Honoring All Attempts | Responding positively to any communication effort, whether it's a gesture, sound, or AAC use. | If your child grunts and looks at the fridge, you respond by saying, "It looks like you want a drink!" and show them the "drink" icon. |
| Wait Time | Pausing for 5-10 seconds after asking a question to give the child time to process and respond. | After asking, "What do you want to play?" you count silently to ten before offering a suggestion or modeling a response on their AAC. |
Ultimately, patience is your most powerful tool. It’s about shifting your own expectations and learning to speak your child’s unique language. When you stop demanding a specific form of communication—like pointing with one finger—and start accepting the movements they can make, like shaking their hand, you build a foundation of trust. That trust is what unlocks their voice.
Why a Professional Diagnosis Is a Critical First Step
When you start to notice that your child communicates differently, it's a huge moment of realization. But it’s the professional diagnosis that truly opens the door to a world of meaningful support. A comprehensive evaluation is so much more than just getting a label—it's the official key that unlocks the resources your child needs, and deserves, to thrive.
The process gives you a complete picture of your child's unique profile of strengths and challenges. A specialist can pinpoint not just the communication differences but also any co-occurring conditions that might be present. For instance, conditions like ADHD or epilepsy are surprisingly common in individuals with non verbal communication and autism, and seeing that full picture is essential for finding support that actually works.
Unlocking Essential Resources
A formal diagnosis is the gateway to critical services. It’s the official documentation you need to secure school accommodations, like an Individualized Education Program (IEP) or a 504 plan, which can provide specialized instruction and classroom supports. It also opens up access to state-funded programs and therapies that might otherwise be completely out of reach.
A diagnosis is not an endpoint. It’s the starting point for ensuring your child is seen, understood, and given access to every tool they need to succeed on their own terms.
Without this crucial step, families often find themselves struggling to get the help they need, trying to navigate a complex system without a clear map. A professional assessment provides that map, outlining a clear path forward based on evidence and your child’s specific needs.
The Importance of a Specialist's Insight
A skilled clinician does more than just run through a checklist of tests. They interpret the subtle nuances of a child’s behavior, carefully separating what might be a developmental delay from a distinct neurotype. They have the training to see past the absence of spoken words to assess underlying cognitive abilities, how much language a child understands, and their motivation to connect with others.
This specialized insight is particularly vital for a population that faces significant hurdles. Think about it: non-verbal communication makes up a huge part of how we all connect, yet our society’s intense focus on speech can lead to profound isolation for non-speaking autistic individuals. When you consider that approximately 40% of children with autism also have epilepsy and nearly 80% have some form of intellectual disability, the need for an expert assessment becomes undeniable. You can find more insights about the complexities of non-verbal autism on healthpolicypartnership.com.
An expert evaluation ensures that support is targeted correctly. It helps differentiate between a child who needs AAC support, one who would benefit from behavioral therapy for co-occurring challenges, and another who simply needs a more accommodating environment to flourish. This clarity prevents families from wasting precious time and resources on strategies that were never going to work.
Ultimately, seeking a professional diagnosis is an act of advocacy for your child. It’s a powerful first move that officially acknowledges your child's reality and arms you with the knowledge and tools to build a supportive, understanding world around them. It shifts your family from a place of uncertainty to one of clarity and action.
How We Provide Clarity with Telehealth Assessments
Figuring out the world of non verbal communication and autism can feel overwhelming, but getting a professional evaluation is the single most important step you can take. It’s how you find clarity and a clear path forward for your child.
At The Sachs Center, we specialize in providing that clarity. Our expert telehealth assessments offer a supportive, effective, and less stressful alternative to traditional in-person testing.
We’ve designed our entire process to reduce the anxiety that often comes with evaluations—for both you and your child. We know from experience that a new, unfamiliar office can be intimidating. It can prevent a child from showing their true self. By conducting assessments virtually, your child gets to stay in the comfort and security of their own home, surrounded by familiar sights and sounds.
A Person-Centered Approach to Virtual Evaluation
Our expert psychologists are incredibly skilled at engaging children and teens remotely. It's a different skillset than in-person work, and they excel at it. They use a thoughtful blend of validated diagnostic tools, structured clinical interviews with parents, and direct observation to build a complete, nuanced picture of your child’s communication style, strengths, and challenges.
This approach lets us see your child in their natural element, which almost always gives us a more accurate and authentic understanding of their abilities. We make a point to focus on what your child can do, not just where they struggle. The goal is to illuminate their potential.
A telehealth assessment isn't just a convenient option; it's a compassionate one. It prioritizes the child's emotional well-being to ensure the diagnostic process is as stress-free and accurate as possible.
Choosing the Right Evaluation for Your Family
We know every family's situation is unique, which is why we offer several assessment options. Taking a moment to understand these choices helps you pick the one that best fits your goals. For an even deeper dive, our detailed guide on the telehealth autism diagnosis process is a great resource.
Here’s a quick look at our primary services:
-
Diagnostic Testing: This is perfect for families who need diagnostic clarity and documentation, often for workplace or initial school accommodations. The evaluation includes a clinical interview and validated assessments, and it concludes with a diagnostic letter from your psychologist.
-
Diagnostic Testing with a Report: This includes everything in the basic package, plus a detailed, four-page report. It gives a much fuller picture of your child's profile, history, and personalized recommendations, making it ideal for coordinating care with other providers like pediatricians or therapists.
-
Neuropsychological Testing: This is our most comprehensive choice. It's for families seeking accommodations on standardized tests (like the SAT, ACT, or GRE) or needing an in-depth evaluation for an IEP or 504 plan. This assessment provides a deep dive into cognitive and academic functioning.
Our psychologists are specialists. They are trained to recognize the nuanced ways autism can present, especially in individuals who have become experts at masking their traits. They look beyond the surface, understanding that what might seem like a lack of communication is actually a rich, nonverbal dialogue.
The final report you receive isn't just a diagnosis. It’s a personalized roadmap with actionable next steps for therapy, school support, and strategies to use at home. By providing this level of detailed insight, we empower you to become your child's most effective advocate, armed with the knowledge to help them truly thrive.
Your Questions About Nonverbal Autism Answered
As a parent or caregiver, navigating the world of nonverbal autism can feel overwhelming, and it’s natural to have a lot of questions. Getting clear, straightforward answers is the first step toward feeling more confident and finding the right path forward for your child.
If My Child Is Nonverbal at Age 4, Will They Ever Speak?
This is one of the biggest worries we hear from parents, but being nonverbal at four is definitely not the end of the story. Research and our own clinical experience show that many children who aren't speaking at this age go on to develop language skills later in childhood. Some even become fluent speakers.
The key is consistent, early support. The immediate goal isn’t just speech—it’s giving your child a reliable way to communicate their needs, wants, and thoughts. This might be through speech, an AAC device, or sign language.
How Can I Tell if My Nonverbal Child Understands Me?
It's a common misconception that a lack of speech equals a lack of understanding. Most of the time, that couldn't be further from the truth. You can get a good sense of their receptive language skills by observing their actions.
Do they follow simple directions like, "get your shoes"? Do they look up when you say their name? If you point to a picture in a book and name it, do they look? These are all signs of understanding.
Many nonverbal children understand far more than they can express. Always presume competence—assume they understand, and provide them with the tools to show you what they know. A comprehensive evaluation can specifically assess these skills.
Are Telehealth Assessments Actually Effective for Nonverbal Kids?
Absolutely. Not only are they effective, but they are often a better option for the child. Our experienced psychologists are experts at engaging children remotely using a mix of parent interviews, live observation, and validated assessment tools designed for a virtual setting.
Think about it: an evaluation in their own comfortable, familiar home environment often gives us a more authentic picture of their abilities than a strange, new office ever could.
What’s the First Step if I Think My Child Might Have Autism?
The single most important first step is to schedule a professional diagnostic evaluation with a specialist who has deep experience in neurodevelopmental conditions.
An accurate diagnosis is the key that unlocks everything else. It’s what you need to access the right therapies, school supports, and other resources that are designed for your child's specific profile of strengths and needs.
Here at the Sachs Center, we specialize in providing that diagnostic clarity through expert telehealth assessments. If you’re ready to get a deeper understanding of your child and find a personalized path forward, learn more and book an evaluation today.