The relationship between autism and OCD is a really important one to understand, mainly because they show up together so often and create some tricky situations for diagnosis and support. While both can involve repetitive behaviors, the reasons behind those behaviors are worlds apart. Getting that distinction right is everything when it comes to effective care.
The Hidden Connection Between Autism and OCD
At first glance, Autism Spectrum Disorder (ASD) and Obsessive-Compulsive Disorder (OCD) can look surprisingly alike. Both can involve repetitive actions, a deep need for routine, and an intense focus on certain things. But these surface-level similarities often hide a more complex connection that needs a closer look.
Think of it like trying to tune into a radio station, but there’s another station broadcasting on a nearly identical frequency. You get a lot of static and overlap, making it hard to hear either broadcast clearly. This “diagnostic static” is why untangling autism from OCD can be such a challenge for individuals, families, and even experienced clinicians.
Understanding the Co-occurrence
The link between these two conditions isn’t just a coincidence; it's statistically huge. Research shows that autistic individuals are far more likely to also have OCD than the general population. One analysis found that the prevalence of OCD in autistic children and teens is a staggering 11.6%.
Let that sink in: out of every 100 kids on the spectrum, about 12 are also fighting a daily battle with OCD. That's a rate five to six times higher than what we see in neurotypical youth. You can find more insights on this comorbidity from the International OCD Foundation (IOCDF).
This high rate of co-occurrence highlights a critical need for awareness. Without it, the distressing symptoms of OCD can easily be brushed off as just “part of the autism,” a frustrating phenomenon known as diagnostic overshadowing. This mistake can prevent someone from getting the specific help they need to manage the anxiety-fueled cycle of OCD.
The real challenge is figuring out the "why" behind a behavior. Is a repetitive action a source of comfort and a way to self-regulate (autism), or is it a desperate attempt to quiet an intrusive, anxiety-producing thought (OCD)?
To make this distinction clearer, let's look at a side-by-side comparison.
Autism vs OCD Quick Overview
This table breaks down some of the core differences and similarities between Autism Spectrum Disorder (ASD) and Obsessive-Compulsive Disorder (OCD) at a glance.
| Feature | Autism Spectrum Disorder (ASD) | Obsessive-Compulsive Disorder (OCD) |
|---|---|---|
| Core Motivation | Behaviors are often driven by sensory needs, self-regulation, or genuine interest. They are typically a source of comfort or enjoyment. | Behaviors (compulsions) are driven by a need to reduce anxiety or prevent a feared outcome caused by intrusive thoughts (obsessions). |
| Repetitive Behaviors | Known as "stimming" (e.g., rocking, hand-flapping). These are usually soothing or pleasurable and not linked to a specific fear. | Known as "compulsions" (e.g., checking, washing, counting). These are rigid, ritualistic acts performed to neutralize a specific obsession. |
| Thoughts/Interests | Intense, passionate interests (often called "special interests") that are a source of joy and expertise. | Intrusive, unwanted thoughts or images (obsessions) that cause significant distress, anxiety, or disgust. |
| Need for Routine | A preference for predictability and routine provides a sense of safety and reduces anxiety. Disruption can be upsetting. | A rigid adherence to rituals is a core part of compulsions. Deviating from the ritual causes intense anxiety about a feared consequence. |
| Social Aspect | Differences in social communication and interaction are a core diagnostic feature. | Social difficulties can arise due to the time-consuming nature of compulsions or obsessions related to social situations, but are not a core feature. |
While this table offers a simplified view, it helps illustrate that even when behaviors look similar on the surface, the internal experiences are fundamentally different.
Why Accurate Diagnosis Matters
Finally recognizing that both conditions can be present at the same time is the first, most crucial step. A correct dual diagnosis opens the door to support that is tailored to the individual—honoring their neurotype while directly treating the debilitating cycle of obsessions and compulsions.
It allows for a more compassionate and effective path forward, one where therapeutic strategies don’t accidentally punish autistic traits while trying to address OCD symptoms. For families and adults navigating this overlap, getting this clarity isn't just a minor detail—it's essential for improving day-to-day life. This is where specialized telehealth services can be incredibly helpful, offering expert guidance to sort through this complex diagnostic puzzle from the comfort of home.
Distinguishing Autistic Repetitive Behaviors from OCD Compulsions
At the heart of the confusion between autism and OCD is a simple question with a complex answer: why is this behavior happening? On the surface, an autistic person’s repetitive action and an OCD compulsion can look identical. The internal motivation, however, is what truly separates the two.
Getting this right isn't just an academic exercise—it’s the key to providing the right kind of support. Mistaking a calming autistic behavior for an OCD compulsion can lead to ineffective interventions. On the flip side, overlooking a distressing compulsion can leave someone struggling with intense, untreated anxiety. The "why" is everything.
Ego-Syntonic vs. Ego-Dystonic Behaviors
One of the clearest ways to tell these behaviors apart is by using two key concepts: ego-syntonic and ego-dystonic. They might sound clinical, but they just describe a straightforward emotional reality.
An ego-syntonic behavior feels like a natural part of you. It lines up with your values, desires, and sense of self. For an autistic person, repetitive behaviors like stimming (rocking, hand-flapping) or arranging objects are often ego-syntonic. They’re done to self-soothe, express joy, or create a comforting sense of order. They feel good, or at the very least, they bring relief and regulation.
In contrast, an ego-dystonic behavior feels foreign, intrusive, and unwanted. It goes against your values and causes significant distress. This is the hallmark of an OCD compulsion. The behavior isn't performed for enjoyment but out of a desperate need to neutralize an obsessive thought and the intense anxiety it creates. It feels like a demand from your brain that you must obey to prevent something bad from happening.
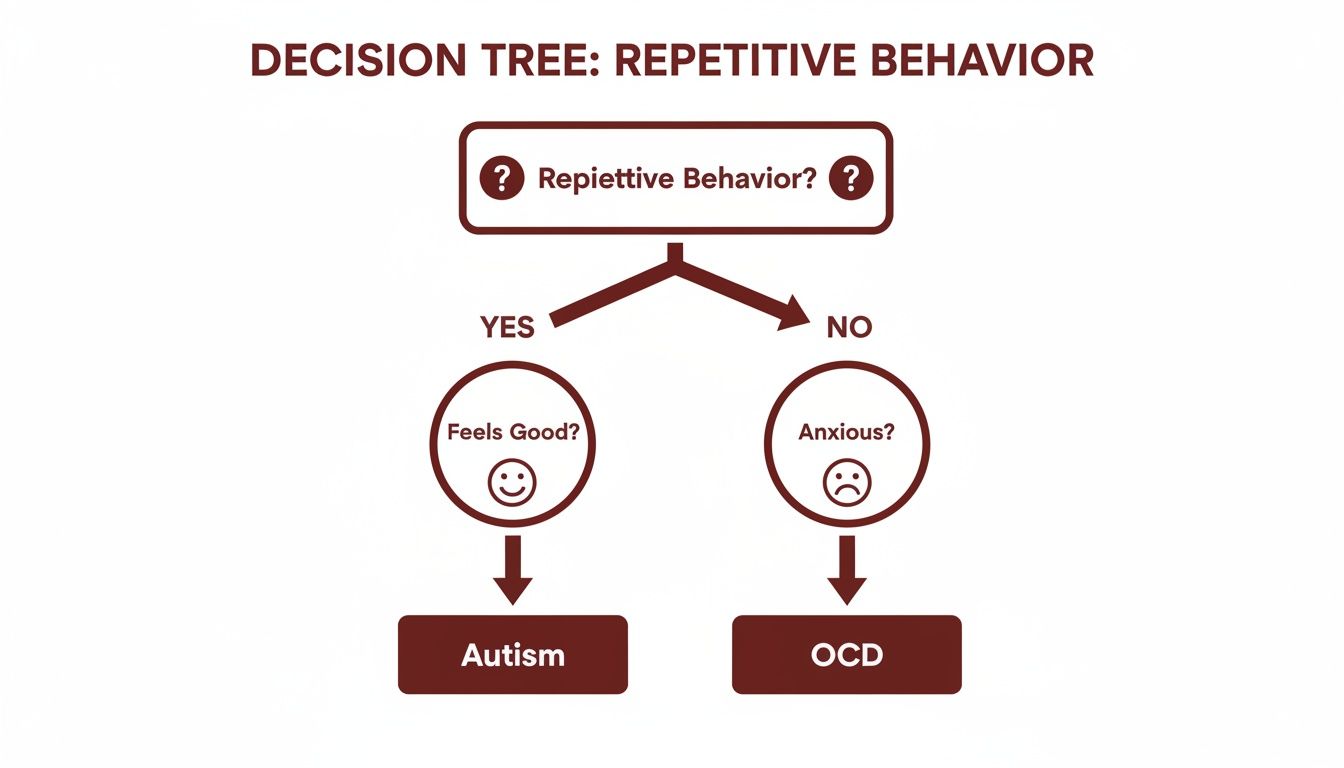
To put it simply, think about the feeling behind the action.
As the chart shows, if a behavior feels good or calming, it points toward autism. If it's driven by anxiety and feels like a command, it's much more likely to be linked to OCD.
Real-World Examples of the Difference
Let's ground these concepts in a real-world scenario. Imagine two children, both meticulously lining up their toy cars.
Scenario 1 (Autism): An autistic child arranges their cars by color and size because they find deep satisfaction in the visual pattern. The process is calming and taps into their special interest in vehicles. If they get interrupted, they might feel frustrated, but the core emotion tied to the activity is comfort and enjoyment. This is ego-syntonic.
Scenario 2 (OCD): A child with OCD lines up their cars in a perfect row because of an intrusive thought that if they don't, something terrible will happen to their family. The act provides no joy; it’s a ritual performed only to relieve overwhelming anxiety for a moment. The driving force is fear, not pleasure. This is ego-dystonic.
This same logic applies to countless other behaviors, from tapping patterns to ordering books.
The core difference isn't the action itself but the internal experience. Autistic repetitive behaviors are often a form of self-expression or self-regulation, while OCD compulsions are a reaction to unwanted, anxiety-provoking obsessions.
Identifying the Motivation Behind the Behavior
For parents, partners, or even individuals trying to understand their own actions, paying attention to the underlying emotions is crucial. When you observe a repetitive behavior, try asking questions that get to the "why."
Here are some key indicators that might suggest a behavior is an OCD compulsion rather than an autistic trait:
- Anxiety-Driven: The person seems highly anxious or distressed before or during the behavior.
- Ritualistic Nature: The behavior must be performed in a very specific, rigid way. Any deviation causes extreme distress.
- No Obvious Pleasure: The person doesn't seem to enjoy the behavior; rather, they appear relieved once it's over.
- Linked to a Fear: The individual may express fears about what will happen if the ritual is not completed correctly.
Recognizing these signs is the first step toward seeking a proper evaluation. Co-occurring autism and OCD requires a nuanced approach, and identifying the ego-dystonic nature of certain behaviors is often the clue that more than just autism is at play.
Challenges in Diagnosing Co-occurring Conditions
Trying to untangle co-occurring autism and OCD is one of the biggest hurdles in neurodivergent care. The symptoms can overlap so much that it creates a kind of diagnostic fog, making it tough for even experienced clinicians to tell where one condition ends and the other begins. This isn't just an academic puzzle; it directly affects whether someone gets the right kind of support.
Think about it: behaviors like sticking to a strict routine, getting really distressed by change, or having repetitive actions are often seen as textbook autism. And they are! But they can also be signs of OCD. This leads to something called diagnostic overshadowing—the more obvious diagnosis of autism can completely hide the co-occurring anxiety disorder, leaving the painful cycle of OCD untreated.
The Problem of Masking and Internal Experience
This gets even trickier when someone has learned to mask their autistic traits, which is especially common in adults and girls. Masking is the exhausting, often subconscious, effort of suppressing natural autistic behaviors to blend in with neurotypical expectations. Someone might force themselves to go with the flow when a routine changes or hide their stimming, but inside, they’re running a marathon.
Now, imagine that person also has OCD. Their inner world becomes a battlefield. They could be fighting off intrusive thoughts that go against their values (ego-dystonic) while trying to appear perfectly calm and collected on the outside. Because the struggle is invisible, their needs often get missed. A standard evaluation that just looks at surface-level behavior might not catch the OCD at all.
This is exactly why a good evaluation has to be more than a simple checklist. It needs to be a deep dive into someone's internal world—to understand the why behind their behaviors and the real emotional cost of just getting through the day.
The Rising Need for Diagnostic Clarity
Getting this right has become more urgent as awareness grows. Since 1970, the reported rate of autism in the US has shot up from around 1 in 5,000 to 1 in 36 by 2023. Within that group, an estimated 17% of autistic individuals also have an OCD diagnosis, a number that dwarfs the rate in the general population. These stats highlight just how critical it is to have assessments that can accurately tell these conditions apart.
This diagnostic complexity can delay a person's understanding of their own neurotype, creating particular challenges for managing a late autism diagnosis in adults. Getting an accurate picture, no matter when it happens, is the key to building a life with the right support.
How Specialized Telehealth Assessments Help
A specialized assessment is the best way to cut through this diagnostic fog. Modern telehealth evaluations are a game-changer here, offering a comfortable, controlled environment for the person being assessed. Being in a familiar space can lower anxiety and reduce the need to mask, which allows for a much more authentic and accurate picture of their experiences.
A solid virtual assessment brings together a few key pieces to achieve that clarity:
- Detailed Developmental History: Clinicians conduct in-depth interviews with the individual and their family (when appropriate) to map out their life experiences. This history is crucial for spotting long-term patterns that point toward either autism, OCD, or both.
- Validated Self-Report Measures: We use standardized, evidence-based questionnaires to gather objective information about specific symptoms. These tools are designed to tease apart the subtle differences between repetitive behaviors, intrusive thoughts, and social communication styles.
- Expert Clinical Observation: A psychologist who specializes in neurodiversity watches for nuances in communication style, thinking patterns, and emotional responses during the virtual session. They’re trained to spot the subtle signs that distinguish autistic traits from OCD symptoms.
By weaving these elements together, clinicians can build a complete, three-dimensional picture of an individual's neurotype. This careful, detailed process is the only way to create a truly effective and personalized support plan. Our guide on how to get tested for autism breaks down what you can expect from a high-quality evaluation.
Adapting Treatments for Individuals with Both Conditions
When it comes to treating Obsessive-Compulsive Disorder in an autistic individual, a one-size-fits-all approach just won't cut it. Standard therapies, while powerful for many, often need significant adjustments to honor the neurotype of someone navigating both autism and OCD. A rigid, unmodified plan can be ineffective at best and deeply distressing at worst.
The real goal here isn't to change autistic traits. It's about tackling the debilitating anxiety and intrusive thoughts that OCD brings to the table. This requires a delicate balance—a true therapeutic partnership that respects sensory needs, communication styles, and the individual's unique way of experiencing the world. Without that foundation, even the most evidence-based treatments are likely to miss the mark.
Modifying the Gold Standard: Exposure and Response Prevention
Exposure and Response Prevention (ERP) is widely seen as the gold standard for OCD treatment. The therapy involves gradually facing fears (exposure) without giving in to the usual compulsive rituals (response prevention). Over time, this teaches the brain that the anxiety will eventually fade on its own without the compulsions.
But applying standard ERP to an autistic person requires careful, neurodiversity-affirming modifications.
Think of it like calibrating a very sensitive instrument. You can’t just force it to work; you have to adjust it with precision and care. For autistic individuals, this calibration involves several key changes:
- Pacing and Gradual Exposure: The whole process needs to be slower and more predictable. Rushing into exposures can easily trigger sensory overload or an autistic shutdown, which is the opposite of productive.
- Incorporating Special Interests: A skilled therapist can weave a person's deep, passionate interests into the therapy to make it more engaging and less threatening. For example, if someone is afraid of germs, an exposure might involve a favorite fictional character "battling" the germs.
- Addressing Sensory Sensitivities: An exposure that seems perfectly fine for a neurotypical person could be completely overwhelming for someone with sensory sensitivities. The therapist must consider how sounds, textures, or lights might amplify distress during an exercise.
- Clear and Concrete Language: A lot of therapy-speak is abstract, which can be confusing. All explanations and instructions need to be direct, literal, and often supported by visual aids to make sense.
This adapted approach makes sure the therapy hits its target—the OCD—without clashing with the person's core autistic experience.
Tailoring Cognitive Behavioral Therapy
Cognitive Behavioral Therapy (CBT) is another fantastic tool, often used right alongside ERP. It’s designed to help people spot and challenge the unhelpful thought patterns that fuel their obsessions. When working with an autistic person, CBT also needs some thoughtful adjustments to really connect.
The key is moving from the abstract to the concrete. Instead of just talking about a vague feeling like "anxiety," a therapist might use a visual thermometer or a feelings wheel to help the individual pinpoint and rate their emotional state with more clarity.
This concrete, hands-on approach makes the internal work of CBT far more accessible. By grounding abstract ideas in tangible, visual tools, therapists can help autistic individuals build the skills to recognize and reframe OCD-driven thoughts without causing extra confusion or frustration. You can learn more about the fundamentals in our guide on what Cognitive Behavioral Therapy is.
An Integrated and Compassionate Approach
Ultimately, the most successful treatment for co-occurring autism and OCD is an integrated one. It’s a blend of modified ERP and CBT, all grounded in a deep, compassionate understanding of autism. This might also involve other supportive strategies.
Medication, for example, is sometimes considered to help manage the intense anxiety from OCD, which can open the door for the therapeutic work to really begin. Building skills in emotional regulation and sensory management can also provide a stronger foundation for tackling OCD symptoms directly. For some, Art Therapy for Stress Management can offer a powerful, non-verbal way to process difficult emotions.
The single most important element, though, is a collaborative spirit. Effective therapy for dually diagnosed individuals is never about "fixing" them. It’s about giving them the right tools, in the right way, so they can reduce the distress from OCD and live a fuller, more authentic life.
Practical Strategies for Daily Life
When you’re dealing with both autism and OCD, daily life requires a delicate balance. It's less about strict behavior management and more about finding a middle ground—one that respects the autistic need for routine while gently pushing back against the anxiety-fueled demands of OCD. The real goal is to build resilience and lower distress, not to fundamentally change who someone is.
For parents and adults alike, the key is to look beyond the behavior and understand the "why" behind it. Is that rigid morning routine a source of calm and predictability in a chaotic world? Or is it a ritual driven by a terrifying, intrusive thought? Knowing the difference is the first step toward building strategies that actually work.
Creating a Supportive Home for a Neurodivergent Child
A supportive home environment is everything for a child navigating the complexities of autism and OCD. It needs to be a safe space that honors their sensory needs while creating small, manageable opportunities to build flexibility.
A great tool here is a visual schedule, which many autistic kids already use. The trick is to adapt it for OCD by intentionally building in flexibility. Instead of a rigid, down-to-the-minute plan, include "choice time" or even "surprise" slots. This helps your child learn to tolerate small changes in a controlled way, which is a fantastic way to gently challenge OCD’s need for absolute certainty.
Another crucial strategy is co-regulation. When a child is spiraling with anxiety, their nervous system is in overdrive. Before you address the compulsive behavior, help them feel calm and grounded first.
- Validate Their Feelings: Try saying, "I see how scared you are right now. It feels like you absolutely have to do this."
- Offer Sensory Comfort: A weighted blanket, a tight hug, or a quiet corner can help their body feel safe again.
- Model Calm Breathing: Take slow, deep breaths with them. Your own calm can be contagious and help their nervous system settle down.
When you prioritize connection over compliance, you build a foundation of trust. This makes it much easier for your child to engage in therapies like Exposure and Response Prevention (ERP), because they see you as an ally in their corner, not just someone enforcing rules.
Strategies for Autistic Adults with OCD
If you're an adult managing both autism and OCD, your journey is often about self-advocacy and finding what works for you. One of the biggest hurdles is learning to tell the difference between a helpful autistic routine and a harmful OCD compulsion. A routine makes your life easier and less stressful; a compulsion might offer a moment of relief, but it ultimately makes your world feel smaller.
It's vital to develop stress management techniques that align with your sensory profile. If traditional mindfulness feels like too much, try these alternatives:
- Auditory Grounding: Put on noise-canceling headphones and listen to a favorite song, focusing only on the bassline or a single instrument.
- Tactile Grounding: Carry a small, smooth stone or a piece of soft fabric in your pocket. Holding it when you feel anxious can be incredibly centering.
- Visual Grounding: Engage with something visually predictable and calming, like watching a lava lamp or organizing your bookshelf by color.
Self-advocacy is another powerful tool. This might look like explaining to your partner why you need a quiet, uncluttered space after a long day, or asking for workplace accommodations that reduce sensory overload. When you’re less overwhelmed, you’re less vulnerable to OCD flare-ups.
Communicating your needs isn’t being difficult; it’s a necessary part of managing your well-being. By proactively shaping your environment, you can reduce the triggers that fuel both autistic burnout and OCD, empowering yourself to live a fuller life.
How Specialized Telehealth Evaluations Provide Clarity
For many neurodivergent people, the thought of a clinical evaluation is enough to cause serious stress. An unfamiliar office, bright lights, and intense social pressure can make it almost impossible to give an authentic picture of who you are. This is exactly where telehealth has become a game-changer for untangling the complexities of autism and OCD.
Virtual assessments mean you can participate from the comfort and safety of your own home. Being in a familiar setting naturally lowers anxiety and reduces the need to mask, which allows clinicians to see a much clearer, more accurate version of your experiences. When that environmental stress is gone, the real diagnostic picture can finally come into focus.
What a Comprehensive Virtual Evaluation Involves
A specialized virtual evaluation is so much more than a simple video call. It's a carefully structured process designed to gather detailed information from multiple angles, ensuring a thorough and reliable assessment. Our clinicians use a blend of validated tools and insightful conversation to get to the heart of what's really going on.
The process usually includes:
- In-Depth Clinical Interviews: The psychologist will spend significant time talking through your developmental history, current struggles, and specific examples of repetitive behaviors or intrusive thoughts. This personal narrative provides critical context that a simple checklist could never hope to capture.
- Validated Self-Report Measures: You’ll complete evidence-based questionnaires designed to measure traits related to both autism and OCD. These tools add objective data to the picture, helping differentiate between symptom types.
- Expert Observation: A specialist trained in neurodiversity watches for communication styles, thought patterns, and emotional responses during the session. They are skilled at spotting the subtle cues that help distinguish autistic traits from OCD symptoms.
By weaving together your personal history, objective data, and expert observation, a telehealth evaluation builds a complete, three-dimensional view of who you are. This approach is essential for accurately diagnosing co-occurring conditions.
From Evaluation to Actionable Support
After the evaluation, all the findings are pulled together into a document that offers both diagnostic clarity and a clear path forward. This isn't just about getting a label; it’s about creating a roadmap for support. Depending on what you need, this can take a couple of different forms. You can find more details by exploring our options for telehealth neuropsychological testing.
Different reporting options are available for different purposes:
- A diagnostic letter is a concise document that confirms a diagnosis. It’s often used to request accommodations at work or to share with a primary care doctor for medication management.
- A comprehensive report is a more detailed, four-page overview. It includes your full history, a breakdown of your challenges, and personalized recommendations, creating a holistic guide for coordinating care with therapists and other providers.
This process ensures that you don’t just leave with answers, but with practical, actionable steps to improve your quality of life.
Unpacking Common Questions About Autism and OCD
When you're trying to understand the connection between autism and OCD, a lot of questions can come up. It's a complex area, and it's natural to feel a bit lost. Let's clear up some of the most common points of confusion.
Can a Person Have Both Autism and OCD?
Yes, absolutely. In fact, it's far more common than you might think. We know from research that OCD shows up much more often in autistic individuals than it does in the general population.
The real challenge, however, isn't whether they can exist together, but how to tell them apart. Both can involve repetitive behaviors and a need for routine, which can look very similar on the surface. This is why a specialized assessment is so important to get an accurate picture.
What Is the Difference Between a Special Interest and an Obsession?
This is a fantastic and crucial question. The biggest difference comes down to the feeling behind the focus.
An autistic special interest is something that brings genuine joy, comfort, and a sense of expertise. It's what we call ego-syntonic—meaning it feels like a core, positive part of who you are.
On the other hand, an OCD obsession is an unwanted, intrusive thought that brings on a wave of anxiety or distress. It’s ego-dystonic, feeling foreign and upsetting. The person then feels compelled to perform an action (a compulsion) to get some relief from that awful feeling.
A special interest is a source of joy; an obsession is a source of dread. Getting this right is fundamental to identifying when OCD is co-occurring with autism.
Is Treatment Different If Someone Has Both Conditions?
Yes, the treatment approach has to be thoughtfully adapted. The gold-standard treatment for OCD is Exposure and Response Prevention (ERP), but you can't just apply it in the standard way for an autistic person.
A modified approach is essential. This means the therapist must respect sensory sensitivities, use clear and concrete language, and maybe even find ways to incorporate special interests into the therapy itself. Most importantly, the goals of therapy should never be about "fixing" or reducing core autistic traits—it's about targeting the OCD in a way that works for a neurodivergent brain.
If you or a loved one are navigating these complexities, getting a clear and accurate diagnosis is the first step. The team of experts at the Sachs Center specializes in precisely these kinds of nuanced evaluations. Our telehealth services are designed to compassionately and accurately diagnose co-occurring conditions like autism and OCD.
Learn more about our approach and book an evaluation.