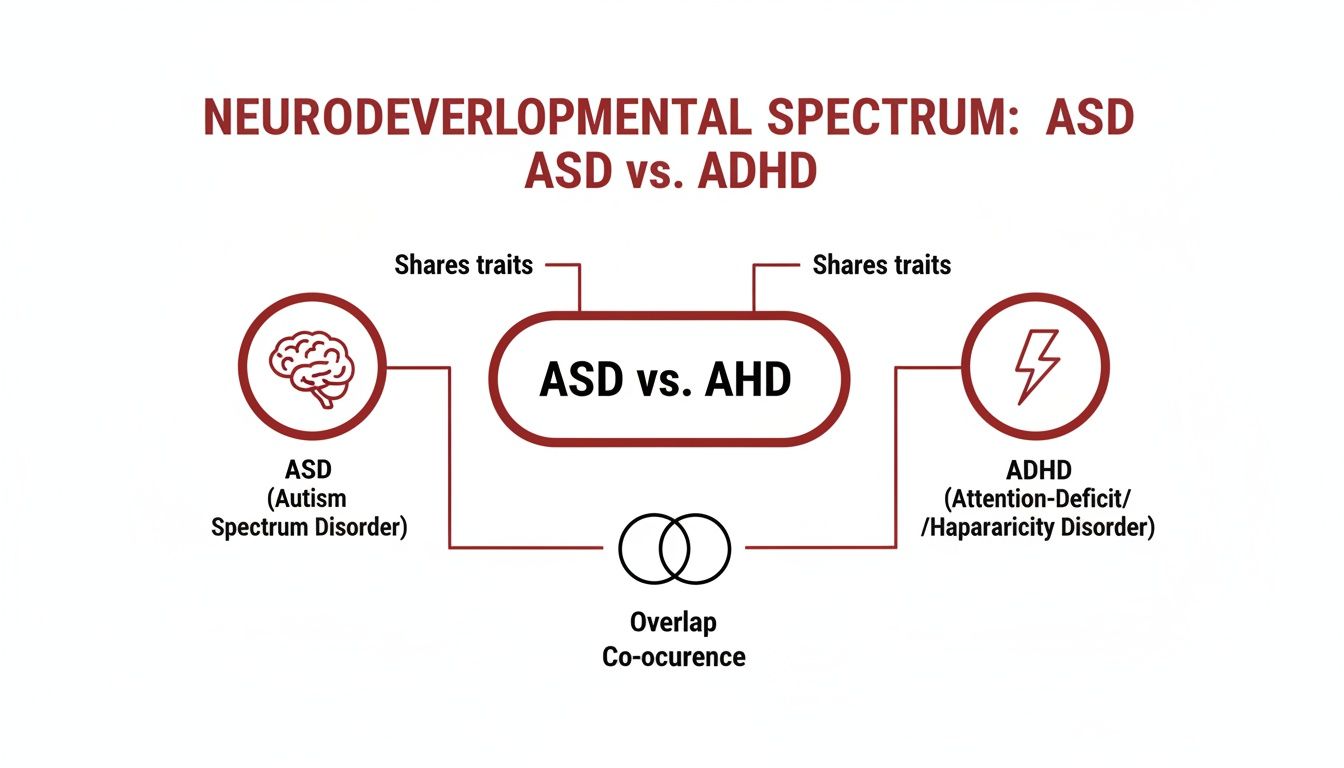
At their core, the fundamental differences between ASD and ADHD come down to their primary challenges. Autism Spectrum Disorder (ASD) is mainly defined by difficulties with social communication and the presence of restricted, repetitive behaviors. On the other hand, Attention-Deficit/Hyperactivity Disorder (ADHD) centers on persistent patterns of inattention and/or hyperactivity-impulsivity that disrupt daily life.
Clarifying the Neurodevelopmental Divide
Both ASD and ADHD are neurodevelopmental conditions, meaning they originate in early childhood and impact how the brain wires itself. They are, however, distinct diagnoses. The confusion often comes from the fact that their outward signs can look remarkably similar, making it easy to misinterpret them without a professional eye.
A big part of this overlap is how both conditions can create significant hurdles with executive functioning—those essential mental skills we rely on for planning, staying organized, and managing self-control. This is why someone with either condition might struggle with daily tasks, emotional regulation, or social situations.
Key Distinctions at a Glance
To really get a handle on the ASD vs. ADHD comparison, it helps to see their main characteristics side-by-side. The table below breaks down the fundamental distinctions in how each condition usually shows up, offering a much clearer picture.
ASD vs ADHD at a Glance Key Distinctions
| Characteristic | Autism Spectrum Disorder (ASD) | Attention-Deficit/Hyperactivity Disorder (ADHD) |
|---|---|---|
| Primary Challenge | Social-communication deficits and restricted/repetitive behaviors. | Pervasive inattention, hyperactivity, and/or impulsivity. |
| Social Interaction | Difficulty interpreting non-verbal cues, understanding social rules, and reciprocity. | Challenges often stem from inattention (missing cues) or impulsivity (interrupting). |
| Focus Pattern | Intense, narrow focus on special interests (hyperfocus); difficulty shifting attention. | Difficulty sustaining attention on non-preferred tasks; easily distracted. |
| Routine & Change | Strong preference for predictability and routine; change can cause significant distress. | Often craves novelty and can become bored with routine; may be spontaneous. |
| Communication Style | May be literal in interpretation and expression; can have scripted or formal speech. | Often characterized by rapid, tangential speech or frequent topic changes. |
Breaking it down this way really highlights how the underlying drivers of behavior differ, even when the behaviors themselves look similar on the surface.
Understanding Prevalence and Co-Occurrence
It's also useful to look at how common these conditions are. Autism Spectrum Disorder affects about 1 in 127 people worldwide. In contrast, ADHD impacts a much larger group—around 11% of U.S. children and 3-4% of adults globally. These numbers alone show why getting the diagnosis right is so critical for connecting people with the right kind of support.
Despite being separate conditions, it's quite common for them to co-occur, a profile that's become known as AuDHD. People with AuDHD navigate a unique blend of traits from both neurotypes, like the classic internal tug-of-war between an autistic need for routine and an ADHD drive for novelty. It’s a common question to ask is ADHD a form of autism, but they are recognized as separate, though frequently overlapping, diagnoses. This complexity is exactly why a thorough, nuanced evaluation is absolutely essential.
A Detailed Comparison of ASD and ADHD Symptoms
While the definitions give us a starting point, the real story of ASD vs. ADHD unfolds in the nuances of daily life. The most critical question isn't what a person is doing, but why they're doing it.
Take a busy party, for example. Someone with ADHD and an autistic person might both find it difficult, but their internal experiences are worlds apart. The person with ADHD might miss social cues because their attention jumped to a fascinating conversation across the room, or they might impulsively interrupt someone to share an exciting thought. For the autistic person, the struggle often comes from the exhausting mental work of trying to decode sarcasm, body language, and all the other unwritten rules of social interaction.
This difference in the "why" is everything when it comes to getting an accurate diagnosis.
This diagram is a great way to visualize where the two conditions stand apart and where they meet.
As you can see, there’s a clear separation between the core traits, but also a significant overlap where symptoms can look similar or even coexist.
Focus and Attention Patterns
One of the starkest contrasts lies in how attention works. ADHD is famously marked by a struggle to keep focus, especially on anything that isn't intensely interesting. The ADHD brain is on a constant hunt for dopamine, which can make boring or repetitive tasks feel almost physically painful.
Autism, on the other hand, is often associated with a deep, powerful focus on specific topics, sometimes called special interests. This goes far beyond a simple hobby; it's a profound passion that can lead to an incredible depth of knowledge. While an autistic person can certainly get distracted, their attention is often narrow and deep, whereas the ADHD brain tends to be broad and constantly scanning its environment.
The core difference often comes down to control and content. An ADHD hyperfocus is usually sparked by a new, exciting interest and can feel a bit random. Autistic hyperfocus is more systematic and often tied to long-standing special interests, providing a deep sense of comfort and order.
Communication and Interaction Styles
Communication styles also provide major clues in the ASD vs. ADHD puzzle. Someone with ADHD might talk a mile a minute, leap between topics, or finish other people’s sentences. Their communication is often driven by impulsivity and a brain that’s moving at lightning speed.
In contrast, autistic communication is typically more literal and direct. There’s often a preference for clear, straightforward language and a real difficulty with the vague, unwritten rules of small talk. An autistic person might not intuitively shift their communication style for their audience, using the same precise tone with a close friend as they would in a formal presentation.
Let's look at a quick scenario:
- ADHD Example: In a work meeting, the person with ADHD might suddenly interrupt with a brilliant idea that just struck them, completely derailing the conversation. It’s not meant to be rude—it’s a desperate attempt to grab the thought before it vanishes.
- ASD Example: In that same meeting, the autistic person might point out a factual inconsistency in the presenter's slides. The goal isn't to undermine the speaker but to correct the information, because accuracy and detail are fundamentally important to how they process the world.
Routines and Sensory Experiences
How a person responds to routines and sensory input is another key differentiator. The autistic brain often finds immense comfort in predictability. Routines create a sense of safety and reduce the mental energy required to navigate a chaotic world, so an unexpected change in plans can be incredibly distressing.
For many with ADHD, routine is the enemy. It feels restrictive and boring. The brain's constant craving for novelty means that spontaneity is energizing, while rigid schedules are a struggle to follow.
Sensory processing is also a huge piece of the puzzle. While both conditions can involve sensory sensitivities, it is a core diagnostic criterion for ASD. An autistic person might be hypersensitive to sounds, light, or the texture of their clothes to the point of physical pain or complete overwhelm. For a deeper dive, it’s worth exploring the concept of sensory integration.
People with ADHD can also have sensory issues, but it often connects back to attention (not noticing a tag is itchy until it’s unbearable) or hyperactivity (seeking out intense sensory feedback). These subtle distinctions are vital for anyone trying to understand the complex relationship between these two conditions.
Exploring the Overlap of AuDHD and Co-Occurring Conditions
The line between ASD and ADHD can get pretty blurry, especially when you realize how often they show up together. When someone meets the diagnostic criteria for both Autism Spectrum Disorder and Attention-Deficit/Hyperactivity Disorder, we call it AuDHD. This isn't just about having two separate conditions; it's a completely unique neurotype with its own distinct mix of strengths and challenges.
Understanding AuDHD is so important because the two conditions create a complex internal tug-of-war. The traits don't just sit side-by-side—they interact, often pulling you in opposite directions. This constant internal friction can be one of the most confusing and exhausting parts of navigating a dual diagnosis.
The Internal Conflict of AuDHD
The core struggle of AuDHD often comes from trying to manage completely contradictory impulses. This can make it incredibly difficult to find strategies that actually work consistently.
Take the classic battle between routine and novelty. The autistic part of the brain thrives on structure and predictability, finding a deep sense of comfort in knowing what comes next. An unexpected change can feel jarring and deeply unsettling. At the exact same time, the ADHD brain is chasing dopamine, which it gets from new, stimulating experiences, making any kind of routine feel painfully dull and confining.
“I often feel like a living contradiction. I want order but cannot maintain it. I want to be systematic and precise but struggle with it, which leaves me constantly feeling not good enough (to my own standards) and like I can never quite ‘get there.’” – Samantha, Australia
This dynamic often creates a frustrating cycle: an intense, autistic-driven desire to create perfectly organized systems, followed by an ADHD-driven inability to maintain them due to executive function challenges or the sheer need for something new. It's a constant push and pull between a deep need for stability and an equally powerful drive for spontaneity.
Social and Emotional Dynamics
The social experience for someone with AuDHD is also uniquely complicated. You might crave social connection (driven by ADHD impulsivity or a passionate interest) but find the actual work of socializing to be overwhelming and draining (a common autistic trait). This can lead to a pattern of enthusiastically making plans, only to feel too depleted to actually follow through.
Emotional regulation is another huge hurdle, with both conditions turning up the dial on emotional intensity, but in different ways.
- ADHD often contributes quick, intense emotional reactions due to impulsivity and challenges with emotional control. Rejection sensitivity dysphoria is a very common experience.
- ASD can lead to emotional overwhelm from sensory overload or social confusion, which might result in meltdowns or shutdowns.
Put them together, and a person might experience rapid, intense emotional shifts that are hard for even them to understand or manage. This only adds another layer of complexity to their inner world and their relationships.
The Importance of a Dual Diagnosis
Recognizing how often these two conditions co-occur is absolutely essential for getting an accurate diagnosis and effective support. The rate of ADHD is significantly higher among autistic individuals than in the general population. In fact, research shows that 27% of autistic adults without an intellectual disability also have ADHD. That number jumps to 40% for those with an intellectual disability. You can explore the findings on comorbid conditions to see just how significant this overlap is.
This high rate of comorbidity is precisely why a surface-level assessment just won't cut it. A clinician needs the expertise to distinguish between overlapping symptoms and identify the distinct patterns of each condition. For instance, are social difficulties coming from a fundamental challenge with reading social cues (ASD), or are they the result of inattention and impulsivity (ADHD)? In AuDHD, the answer is often both.
Because it's so complex, seeking a specialized evaluation is critical. A comprehensive assessment can untangle the threads of both conditions, leading to a diagnosis that truly reflects what a person is experiencing. You can learn more about combined autism and ADHD evaluations to see how a specialized process is designed to address this unique profile. An accurate AuDHD diagnosis is the key to unlocking support strategies that honor both the need for structure and the drive for flexibility.
How ASD and ADHD Present Differently Across Genders and Ages
When we think of ADHD, the classic picture is often a hyperactive young boy. For autism, it might be a non-verbal boy fixated on trains. But these stereotypes are incredibly narrow and miss the mark on how these conditions actually show up across different ages and genders. The reality is that the expression of both ASD and ADHD is shaped heavily by developmental stages and societal pressures.
This is especially true for girls and women. They often develop sophisticated coping mechanisms to hide their traits, a phenomenon known as masking. The intense pressure to conform socially can lead them to consciously or unconsciously camouflage their neurodivergent behaviors, which is a major reason they've been historically underdiagnosed. Understanding these less obvious presentations is a critical piece of the ASD vs ADHD puzzle.
Gendered Presentations and the Impact of Masking
For many girls, neurodivergent traits turn inward rather than exploding outward. This quieter presentation is often misinterpreted by parents, teachers, and even clinicians, leading to missed diagnoses or the wrong ones.
Take ADHD. A girl might not be climbing the classroom furniture. Instead, her inattentive-type ADHD could look like quiet daydreaming, earning her the label "spacey." She might struggle with social dynamics simply because she's missing conversational cues. Her hyperactivity is often more subtle—fidgeting with her hair, doodling with intensity, or just feeling a constant internal buzz of thoughts.
Autistic girls often become masters of social mimicry. They might meticulously study their peers to learn and replicate facial expressions, vocal tones, and social scripts just to fit in. This camouflaging is exhausting but effective at keeping them off the diagnostic radar. While a boy might be open about his special interest, a girl may choose a more "socially acceptable" one, like a popular book series, to avoid standing out.
Masking isn't a sign of 'mild' symptoms; it’s a testament to the immense energy spent navigating a world not built for the neurodivergent brain. This constant performance is a major contributor to anxiety, depression, and burnout, especially in women diagnosed later in life.
How Symptoms Evolve From Childhood to Adulthood
Just as gender shapes how ASD and ADHD present, so does age. The core neurodivergence doesn't change, but the way it manifests adapts to the different demands of each life stage. What looks like one thing in a five-year-old can be completely transformed in a thirty-year-old.
Recognizing this evolution is the key to identifying these conditions in adults who were missed as children.
Hyperactivity to Restlessness: The boundless physical energy of a child with ADHD often morphs into a persistent feeling of internal restlessness in adults. An adult might not be running around the office, but they may constantly tap their foot, need to get up and walk around, or feel a relentless need to stay busy.
Meltdowns to Autistic Burnout: Childhood meltdowns, often triggered by sensory or emotional overwhelm, can become less frequent but more profound in adulthood. Years of masking and navigating a stressful world can lead to autistic burnout—a state of intense physical, mental, and emotional exhaustion where coping skills seem to temporarily vanish.
Inattention to Executive Dysfunction: A child's trouble paying attention in class becomes an adult's daily battle with executive dysfunction. This shows up as difficulty planning long-term projects, chronic disorganization at home and work, poor time management, and a frustrating inability to initiate or complete important tasks.
Understanding these developmental shifts is vital. An adult seeking an evaluation might not see themselves in childhood symptom checklists until they reframe them through the lens of their adult experiences. This nuanced view is exactly why it's so important to find a diagnostician who is experienced in the varied and masked presentations of ASD vs ADHD to get a clear diagnosis, no matter your age or gender.
Navigating the Path to an Accurate Diagnosis
Deciding to seek a formal diagnosis for ASD or ADHD can feel like a massive, nerve-wracking step. But just understanding what the process looks like can make it all feel much more manageable. Getting an evaluation isn't about getting a label—it's about gaining clarity, unlocking the right support, and finally having a real framework to understand your own experiences.
The whole journey starts with a comprehensive diagnostic evaluation. This process is designed to build a complete picture of you, connecting your present-day challenges with your developmental history to see if your experiences truly line up with the criteria for ASD, ADHD, or both.
What to Expect During an Evaluation
A quality evaluation is a detailed, collaborative process, not just a quick checklist. To get to an accurate and thoughtful conclusion, it typically involves a few key components.
The cornerstone is always the clinical interview. This is really just a guided conversation where a psychologist will ask about your early childhood, your experiences in school, your work history, social relationships, and the struggles you're facing right now. For adults, this might mean asking a parent or older sibling to share their memories, since symptoms have to be present from childhood to count toward a diagnosis.
After the interview, you'll most likely work through some validated assessment tools. These are standardized, evidence-based questionnaires and self-report forms that help quantify your symptoms and see how they stack up against established diagnostic criteria. This data-driven approach adds a critical layer of objectivity to the clinician's professional judgment.
The real goal of a diagnostic evaluation is to figure out the why behind your challenges. It’s all about distinguishing between overlapping traits to find the root cause, which is the most important step in creating a support plan that actually works.
Choosing the Right Type of Assessment
Not all evaluations are created equal, and the right one for you depends entirely on what you're trying to achieve. It’s really important to understand the difference between a standard diagnostic assessment and a full neuropsychological evaluation, because knowing this can save you a lot of time and money.
A comprehensive diagnostic evaluation is exactly what most adults need when they're seeking clarity. This type of assessment is sufficient for:
- Getting a formal diagnosis for your own personal understanding.
- Obtaining workplace accommodations under the Americans with Disabilities Act (ADA).
- Providing the right documentation to a psychiatrist or primary care doctor for medication management.
On the other hand, a full neuropsychological evaluation is a much more intensive—and expensive—process. This in-depth assessment is specifically required when you need formal academic accommodations for standardized tests (like the SAT, GRE, or MCAT) or to secure an IEP or 504 plan in a school setting. It involves a whole battery of cognitive and academic tests that go way beyond what’s needed for a standard diagnosis. For a deeper dive into what these evaluations cover, you can learn more about professional autism and ADHD diagnosis options.
Understanding this distinction is key. For the vast majority of adults, a standard evaluation provides everything you need to move forward with confidence and get the right support in place.
Choosing the Right Evaluation at The Sachs Center
To make it even clearer, we’ve broken down our evaluation packages to help you decide which path is right for your specific situation and goals.
| Evaluation Type | Best For | Deliverable | Price |
|---|---|---|---|
| Basic Diagnostic Evaluation | Individuals seeking diagnostic clarity for personal understanding or medication management with their provider. | A 1-2 page summary letter with diagnostic findings. | $1,500 |
| Comprehensive Diagnostic Evaluation | Individuals needing a formal diagnosis for workplace (ADA) or college-level accommodations. | A comprehensive 10-15 page report with detailed findings, history, and recommendations. | $3,500 |
| Full Neuropsychological Evaluation | Students requiring documentation for standardized test accommodations (e.g., SAT, ACT, GRE, MCAT) or K-12 school-based support (IEP/504 plans). | An extensive 20-30 page report including cognitive and academic testing results, required by testing boards. | $6,500 |
Ultimately, choosing the right assessment ensures you get the answers and documentation you need without spending more time or money than necessary. If you're unsure, our team can help guide you to the evaluation that best fits your needs.
Comparing Support Strategies and Treatment Approaches
Once a diagnosis is on the table, the conversation shifts to finding the right kind of support—and this is where the paths for ASD and ADHD really diverge. There's no one-size-fits-all intervention. For any strategy to be effective, it has to align with the person's specific neurotype. The goal is always to build skills and create supportive environments, not to "fix" who someone is.
For many with ADHD, a good starting point is often a mix of medication and practical skill-building. Stimulant or non-stimulant medications can be incredibly helpful for managing the core symptoms of inattention and hyperactivity. This often clears up the mental fog, creating the bandwidth needed for other strategies, like executive function coaching, to actually stick.
Tailoring Therapeutic Interventions
Therapy is another huge piece of the puzzle, but the type of therapy matters. Cognitive Behavioral Therapy (CBT) is a common and effective tool for ADHD, helping individuals build practical coping mechanisms for things like procrastination or emotional overwhelm. It's all about reframing thought patterns to change behaviors.
But for autistic individuals, the focus is different. Support is geared more toward navigating the social world and managing sensory needs. While medication might be used for co-occurring conditions like anxiety, it doesn’t address the core traits of autism. Instead, therapies concentrate on building skills and reducing the distress that comes from a world not built for them.
A key distinction in therapeutic approaches is adaptation. Standard CBT can sometimes fall flat for autistic individuals because of its reliance on abstract social concepts. Adapted CBT, which uses more literal language and visual aids, is often far more successful.
This just goes to show how critical it is to find practitioners who truly get the nuances of autistic processing.
Building Strengths and Fostering Well-Being
A modern, strengths-based approach is about moving beyond just managing deficits. It’s about helping people see their neurodivergent traits as assets. This could mean finding a career that celebrates the deep, sustained focus of an autistic person or taps into the creative, out-of-the-box problem-solving of someone with ADHD.
Strong support systems are essential for making this happen. These can look like:
- Psychoeducation: Giving individuals and their families real, detailed information about their neurotype. This cuts down on self-blame and builds genuine self-awareness.
- Skills Coaching: Offering targeted, practical guidance for everyday challenges, whether it's organizing a workspace or getting through a crowded party.
- Community Groups: Connecting with other neurodivergent people offers validation, a shared language, and a powerful sense of not being alone.
When it comes to the classroom, understanding how SEL supports neurodiverse students can provide a roadmap for fostering both well-being and academic growth.
For those with AuDHD, a truly integrated plan is non-negotiable. It has to balance the ADHD brain's need for novelty and stimulation with the autistic brain's need for routine and predictability. This often requires a creative blend of strategies from both worlds, creating a personalized approach that isn't just effective, but affirming.
Still Have Questions About ASD and ADHD?
Working through the differences between ASD and ADHD can feel complex, and it’s natural to have specific questions pop up along the way. Let's tackle a few of the most common ones we hear from people trying to find clarity.
Can You Have Both ASD and ADHD?
Absolutely. In fact, it's quite common for Autism Spectrum Disorder and ADHD to show up together. When they do, this profile is often called AuDHD.
Research shows a really high rate of comorbidity, which just means a significant number of autistic people also fit the diagnostic criteria for ADHD. This is exactly why specialized centers, like ours, provide combined evaluations to make sure we get a complete and accurate picture that truly addresses the unique profile of AuDHD.
Are Online Evaluations for Autism or ADHD Legit?
Yes, they are. When conducted by a qualified psychologist using validated, evidence-based assessment tools, telehealth evaluations are both legitimate and effective. A thorough process that includes a detailed clinical interview and standardized self-report questionnaires can provide a completely valid diagnosis.
This remote approach is a game-changer for accessibility and comfort, especially for anyone who finds a formal, in-person clinical setting stressful. The diagnostic reports that come from these evaluations are recognized for creating treatment plans and getting workplace accommodations.
The real difference in social challenges comes down to the root cause. For someone with ASD, it's often an innate difficulty in processing unspoken social rules and non-verbal cues. For someone with ADHD, social struggles are frequently a side effect of impulsivity, inattention, or emotional dysregulation.
Do I Need a Full Neuropsychological Exam for a Diagnosis?
Not usually, no. For most people seeking a standard diagnosis of ASD or ADHD, a massive neuropsychological evaluation isn't necessary. A comprehensive diagnostic evaluation is typically more than enough to provide personal clarity, access medication, and secure accommodations at work.
However, there are specific times when a full neuropsychological test battery is required, specifically when you're seeking formal academic accommodations. This is the case for standardized tests like the SAT or GRE, or for getting school-based support like an IEP or 504 plan.
Ready to get the clarity you deserve? The team of specialists at Sachs Center provides expert, compassionate telehealth evaluations for ASD, ADHD, and AuDHD. Book your evaluation today and take the first step toward understanding your unique neurotype.